Coronavirus: How the World's Healthcare Workers Are in Peril
Part of the weekly column by The Conversation's international health editors.
The world shut down in March. Schools, industries, amateur and professional sports, entertainment and cultural events, and businesses large and small all ceased operating in a manner so sudden and complete it would have been unimaginable a few months ago.
April began with the acceptance that these efforts to contain the spread of COVID-19 must continue. Millions of people were faced with the realities of having to pay bills, rent and mortgages despite layoffs and shuttered businesses. And on April 2, the pandemic itself passed a couple of grim milestones: more than one million confirmed infections and 50,000 deaths worldwide.
It is the health-care workers who are dealing head-on with the reality of those staggering global statistics. The rest of us can help control the numbers by staying at home and practising social distancing.
This fifth weekly column by our team of international health editors highlights more of the recently published articles from The Conversation’s global network.
Vulnerable heroes
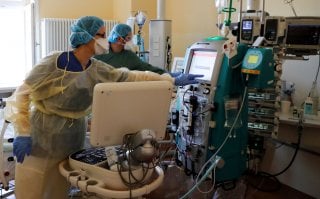
In photos, front-line health-care workers are rendered anonymous by gowns, masks and gloves, like superheroes with secret identities but less glamorous costumes. Unlike their comic-book counterparts, they have no superpowers, not even the dependable tools of vaccines and evidence-based treatments.
And they are frighteningly mortal — as vulnerable as the rest of us to the illness they’re trying to treat.
● Shortage of masks. This makes the growing shortage of personal protective equipment a dire emergency, writes W. Graham Carlos of Indiana University School of Medicine.
● Shortage of ventilators. It’s also very likely that health-care workers will face difficult decisions about which patients get ventilators and intensive care beds. Anthony Wrigley of Keele University, England, explains the ethical choices involved in allocating resources in a crisis situation.
● Shortage of staff. With all hands on deck at hospitals, some facilities are encouraging people still in training or health-care workers from other jurisdictions to help out. However, as Nicole Blay of Western Sydney University and Christine Duffield and Michael Roche of University of Technology Sydney point out, we must be sure that those brought in to help cope with the pandemic are qualified to take on those tasks.
Their work will get harder in many places
The coronavirus continues to spread exponentially around the world, which means that as more people become infected, the virus spreads faster.
● Speed of transmission. Christian Yates of the University of Bath, England, explains the math behind the virus’s exponential spread.
● Examining Indonesia’s high mortality rate. In many regions, the worst is yet to come. While cases in the northern hemisphere are spiking, the first case in Indonesia was only diagnosed on March 2. Since then, the fatality rate in Indonesia has become the highest in Southeast Asia. However, Henry Surenda, of the Eijkman-Oxford Clinical Research Unit, explains three reasons why that fatality rate does not reflect the reality on the ground.
● Unique issues in Africa. SARS-CoV-2 has arrived in Africa later than it did in Asia and Europe, just as SARS did in 2003 and H1N1 did in 2009. Elena Gomez Diaz, from the López-Neyra Institute of Parasitology and Biomedicine, and Israel Cruz Mata, of Instituto de Salud Carlos III, explain why the COVID-19 pandemic in Africa is so worrying (in Spanish).
● Testing decisions. Doyin Odubanjo, executive secretary of the Nigerian Academy of Science, explains why testing is central to the fight against COVID-19, and discusses some of the many factors African countries must consider when making decisions about how to approach testing.
● Who is at risk? Meanwhile, areas already hit hard by the virus are beginning to reckon with the losses. Jean-François Toussaint, from the Université de Paris, and Guillaume Saulière, of the Institut national du sport de l'expertise et de la performance, describe the toll of COVID-19 on vulnerable older populations (in French).
Treatment updates
● Vaccine development. The best way to combat the virus is a vaccine. Kylie Quinn, from RMIT University, and Damian Purcell, of the Peter Doherty Institute for Infection and Immunity, Melbourne, offer an update on the efforts to develop a SARS-CoV-2 vaccine.
● Chloroquine studies. In terms of treatments, there was hope that the malaria medication chloroquine might be a useful treatment for COVID-19. But as Arsène Zongo from the Université Laval, Canada, reports, published studies have not proven its effectiveness (in French).
● Antiviral drugs. Vicente Soriano of Universidad Internacional de La Rioja writes about antiviral medications, which can shorten the duration and severity of symptoms (in Spanish).
Stay informed, stay home, stay six feet away
For the vast majority of us who are not researchers or health-care workers or providing essential services, the best way to help is to stay informed, stay home and stay two metres away from others.
● COVID-19 glossary. You can improve your understanding of what scientists, researchers and health-care workers are talking about with this handy cheat-sheet on coronavirus jargon, provided by Lindsay Broadbent of Queen’s University Belfast.
Many people are looking for practical information about the virus and how to prevent infection. The Conversation’s editors around the globe have recruited experts to answer many of those questions.
● Social distancing rules. The Conversation team in Australia got answers about where people can and can’t go during social distancing from legal experts Brendan Gogarty at the University of Tasmania and Ros Vickers at Charles Darwin University.
● Coronavirus FAQs. Craig Janes, from the University of Waterloo, Canada, patiently answered a long list of questions about how to destroy the virus, how long it persists on surfaces and more.
● Sex and social distancing. But there was still one more question, and we weren’t afraid to ask. Here are the dos and don’ts of sex during social distancing, courtesy of Gonzalo R. Quintana Zunino at Concordia University, Canada.
Get the latest news and advice on COVID-19, direct from the experts in your inbox. Join hundreds of thousands who trust experts by subscribing to our newsletter.
![]()
Patricia Nicholson, Health + Medicine Editor, The Conversation
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Image: Reuters